Tag: #mfc

Welcome to our new General Manager
We would like to extend a very warm welcome to a new member of the MFC management team. Georgina Kearney…
Read More
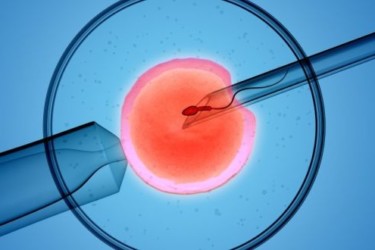
What is the IVF Process?
The IVF process is emotionally intense, physically draining and expensive. But advanced medical knowledge and pioneering lab techniques are making the ‘take-home baby…
Read MoreFertility Preservation in Cancer
The Irish Cancer Society hosted their ‘Living Well with and Beyond Cancer’ 2019 national conference on Saturday September 7th…
Read More
Concern as IVF funding still not in place
Despite the official government announcement last year that €1 million would be allocated for public IVF funding, these funds have…
Read More
SHARP program in Brussels: May 14th-15th
Dr. Helen Spillane of MFC recently took part in a conference at The Centre for Reproductive Medicine of Universitair Ziekenhuis Brussels….
Read More
HFEA report (May 9th 2019): “IVF more popular, successful and safer than ever but reasons for treatment are changing”
The Human Fertility and Embryology Authority has just released its latest report on trends and figures in fertility treatment. Their…
Read More
Boosting male fertility
In at least 50% of cases of male factor infertility, the cause is unknown. A number of lifestyle factors have…
Read More
New Research Funding for MFC Clinician
MFC is delighted to share that our clinical research fellow Dr. Lucia Hartigan recently received research funding from the National…
Read More
Friday, March 8th 2019 – International Women’s Day
We at MFC are celebrating International Women’s Day! This year the campaign theme is #BalanceforBetter, and what better way to…
Read More
- 1
- 2