Tag: #fertility

Launch of the Childhood Cancer Fertility Project
Merrion Fertility Clinic, in collaboration with the Irish Cancer Society, is proud to announce the launch of the Childhood Cancer…
Read More
The Basics of Conception
In this excerpt from her book, MFC Clinical Director, Prof Mary Wingfield, explains the basic biology behind conception and how this…
Read More
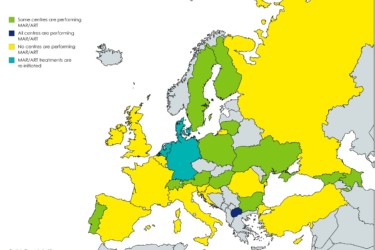
ART In Europe
We know that the cancellation and postponement of treatment due to Covid 19 has brought untold stress and disappointment for…
Read More
Coping During the COVID-19 Pandemic: Message for Our Patients
The Covid-19 pandemic has changed life as we know it. For those patients struggling with infertility, particularly those awaiting treatment,…
Read More
Pre-Implantation Genetic Testing
PGD (Pre-implantation genetic diagnosis) was developed several years ago and is an excellent technique for diagnosing embryos that have…
Read More
Merrion Fertility Clinic’s Top Ten Highlights of the Past Decade
No. 1: Expanded Facility 2010: We moved into our current facility in no.60 Lower Mount Street which gave us the…
Read More
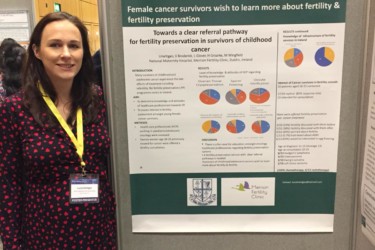
MFC Research at Fertility 2020
Research and clinical staff from Merrion Fertility Clinic presented their findings recently at the Fertility 2020 Conference in Edinburgh….
Read More
Fertility 2020
The 2020 Joint Conference of the Association of Clinical Embryologists, British Fertility Society and the Society for Reproduction & Fertility…
Read More
IVF Add-Ons: Do à La Carte Menus Serve Infertility Patients?
“Add-on” treatments and medications in IVF are highly controversial in the infertility field. At Merrion Fertility Clinic, we believe that…
Read More
- 1
- 2