Tag: #dublin

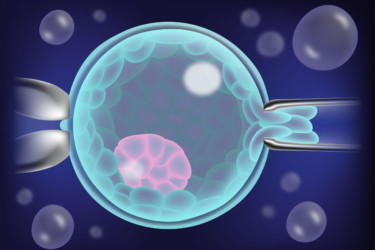
Pre-Implantation Genetic Testing
PGD (Pre-implantation genetic diagnosis) was developed several years ago and is an excellent technique for diagnosing embryos that have…
Read More
What is the IVF Process?
The IVF process is emotionally intense, physically draining and expensive. But advanced medical knowledge and pioneering lab techniques are making the ‘take-home baby…
Read More
IVF Clinics Face New Crackdown on add-on treatments
As a not-for-profit clinic, we at Merrion Fertility Clinic and the National Maternity Hospital are passionate about fairness and making…
Read More
Concern as IVF funding still not in place
Despite the official government announcement last year that €1 million would be allocated for public IVF funding, these funds have…
Read More
SHARP program in Brussels: May 14th-15th
Dr. Helen Spillane of MFC recently took part in a conference at The Centre for Reproductive Medicine of Universitair Ziekenhuis Brussels….
Read More
HFEA report (May 9th 2019): “IVF more popular, successful and safer than ever but reasons for treatment are changing”
The Human Fertility and Embryology Authority has just released its latest report on trends and figures in fertility treatment. Their…
Read More
Boosting male fertility
In at least 50% of cases of male factor infertility, the cause is unknown. A number of lifestyle factors have…
Read More
18th World Congress of the Academy of Human Reproduction 2019
Merrion Fertility Clinic were delighted to participate in the 18th World Congress of the Academy of Human Reproduction, held in…
Read More
“Guaranteed baby or your money back! Too good to be true?”
As a not-for-profit clinic, we at Merrion Fertility Clinic and the National Maternity Hospital are passionate about fairness and making…
Read More
- 1
- 2