Category: News & Events

Abby, Fertility Nurse at Merrion Fertility Clinic, recently featured on the IANO Podcast
We’re delighted to share that Abby, Fertility Nurse at Merrion Fertility Clinic, recently featured on the IANO Podcast alongside hosts…
Read More
Dr. David Crosby on Pathways to Parenthood with Clare McKenna
Our Clinical Director, Dr. David Crosby, recently joined Clare McKenna for episode one of her new mini-series Pathways to Parenthood…
Read More
Merrion Fertility Clinic Launches New Patient Charter
Patient Charter: A Commitment to Excellent Care Merrion Fertility Clinic is thrilled to announce the launch of our new…
Read More
Celebrating 25 Years of Merrion Fertility Clinic
Introduction We are very happy to announce an exciting change in our Clinic that coincides with a significant milestone –…
Read More
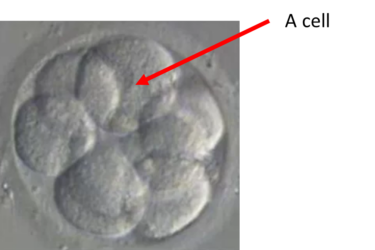
Understanding Embryo Grading
Embryo Development Once your eggs have been collected, the embryology team will become your point of contact for finding out…
Read More
Understanding PCOS: Symptoms, Causes, and Management
What is PCOS?Polycystic Ovary Syndrome, commonly known as PCOS, is a complex and often misunderstood hormonal disorder that can significantly…
Read More
Everything you need to know about the HSE’s publicly funded fertility treatment services
We are delighted to announce that Merrion Fertility Clinic has been selected as an approved provider for publicly funded advanced…
Read More
IUI, IVF & ICSI Explained by Dr Renato
In the video below, our Clinical Lead, Dr Renato Bauman, talks about the fertility treatment options available in the Clinic…
Read More
How does nutrition affect fertility?
This article is based on a webinar on nutrition and lifestyle advice for those trying to conceive given by Orla…
Read More